
Exuding wounds are part of palliative care that are often overlooked. At the same time, they can affect both the patient’s comfort and dignity, and create a more demanding situation for healthcare staff.
Managing wound exudate effectively requires both knowledge and suitable conditions. In this article, we emphasise what exuding wounds can indicate in practice and how dressing selection can improve manageability.
![]()
Around 600,000 – 700,000 deaths are reported yearly in the UK. Many of them live for a long time with illnesses that cannot be cured, such as cancer, cardiovascular disease, dementia and respiratory disease.1 During that time, palliative care makes a big difference. It can help relieve symptoms, reduce suffering, and improve quality of life for both the patient and their loved ones.2
In this context, data from the UK and Canada also show that roughly one quarter of all those who die have such complex needs that they require support from specialised palliative care.3
At the same time, reality often looks quite different. When resources or specialist expertise are unavailable, the responsibility falls on healthcare staff in municipal care, home nursing, or hospital wards.4 Many do an excellent job, but they do not always have the in-depth knowledge needed.
This is also highlighted in the report “Unequal access to specialist palliative care in Sweden” from the Swedish Palliative Care Registry. They also emphasise the importance of pain and symptom assessment.5
![]()
When someone is experiencing long-term pain, it can be difficult to perceive how much they are hurting, so we need to ask actively and trust their responses. Using a pain rating also makes it easier to assess the effectiveness of the steps taken and to indicate whether further action is necessary.
![]()
When discussing palliative care, the emphasis is often on pain, breathing issues, or anxiety. Meanwhile, wounds are a relatively common aspect of end-of-life care, including pressure ulcers, tumour wounds, lymphoedema, or leg ulcers.
This is a situation many people face, and it can be hard to handle without the right support, not least because knowledge and access to wound care support are often limited.6
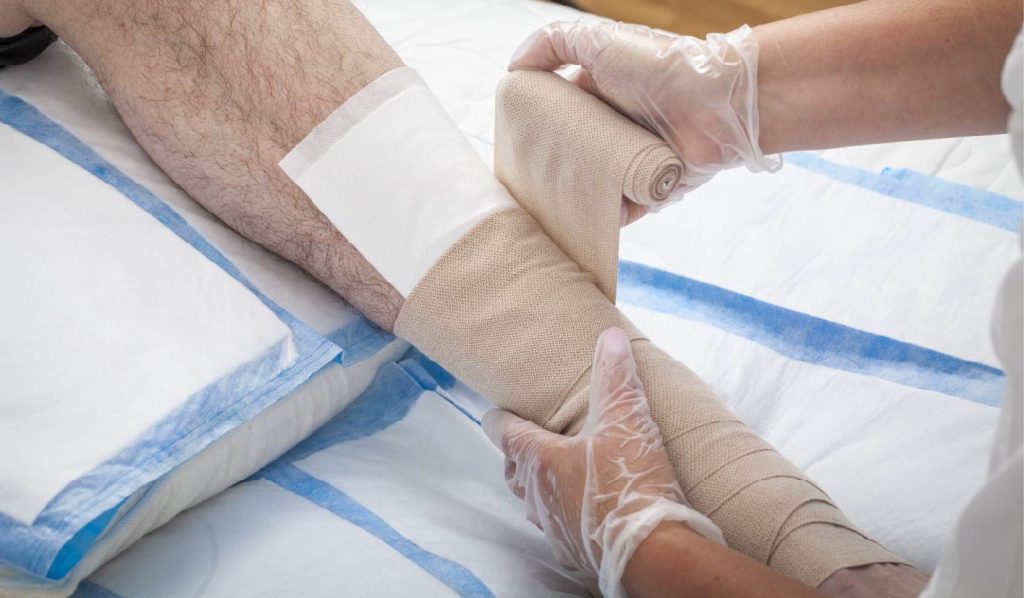
Wound care in palliative treatment also differs from conventional wound management. Here, the aim is not always to heal the wound, but to alleviate symptoms and ensure the best possible quality of life.
Many of these challenges are interconnected and become especially evident in wounds with heavy exudate. Leakage, odour, infection, and pain not only impact the patient’s comfort7 but also their sense of dignity in an already vulnerable situation.8
At the same time, healthcare staff are also impacted. When wound exudate is not managed properly, dressings must be changed more frequently than necessary. This can disturb the patient’s rest, increase discomfort, and create a more stressful work environment.
If a dressing cannot control excess fluid, it must be changed more often than desired and will not effectively manage wound exudate-related issues.
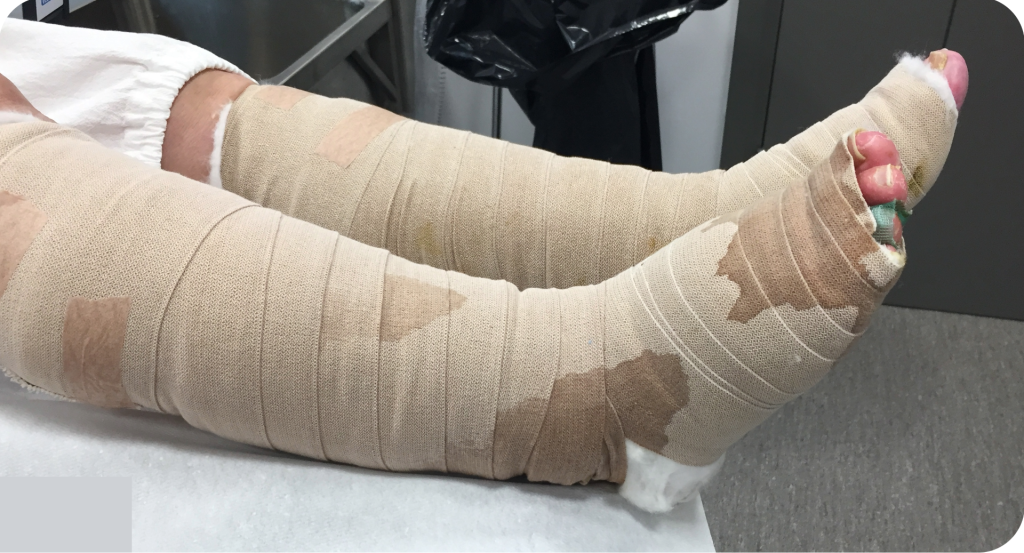
Often, a lack of knowledge about which dressings can handle larger amounts of exudate prevents the treatment from achieving its intended effect. This can make the treatment more reactive than planned, with the focus shifting from preventing consequences to managing them.9

When wound exudate becomes difficult to manage, it is rarely a single problem; instead, it can trigger a chain of consequences. Leakage, skin damage, odour, and frequent dressing changes are often interconnected. At the same time, a wound will often heal well when it maintains an optimal moisture balance – slightly moist, but not too wet.10
In such cases, the choice of dressing becomes a crucial part of the treatment.
The aim is to select a dressing that not only absorbs fluid temporarily but also manages it over a longer period without leaking or damaging the skin around the wound.
For wounds with heavy exudate, a superabsorbent dressing can often be a suitable option to consider, as they are designed to:
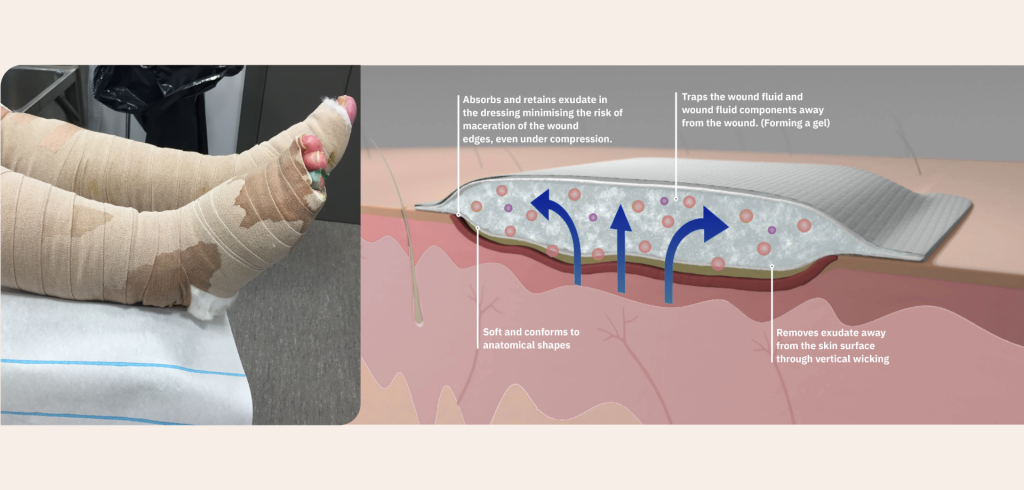
Improved fluid management can reduce the need for frequent dressing changes. This, in turn, helps minimise disruptions for the patient and encourages a more sustainable working environment for healthcare staff.
At the same time, it is essential to remember that there are different types of dressings, and the choice must always be tailored to the wound’s appearance and the patient’s needs.
In palliative care, wound management aims not only at healing but also at reducing discomfort.
Exuding wounds are common but can be difficult to manage without proper knowledge and appropriate dressings. When wound exudate is controlled, it often reduces multiple issues simultaneously for both the patient and healthcare staff.
Selecting the appropriate dressing can be a simple yet impactful change in the treatment that makes a considerable difference.

Experience the difference and compare the outcome with our superabsorbent primary dressing. Designed for comfort and to facilitate a simple wound healing process, it creates optimal healing environments to support clinicians in delivering quality care.
1. Specialised palliative care in Sweden, palliativregistret.se
2. World Health Organisation, Fact sheet Palliativ Care
3. Specialised palliative care in Sweden, palliativregistret.se
4. Specialised palliative care in Sweden, palliativregistret.se
5. Reference guide for nursing assistants; Svenska Palliative Registret.
6. Palliative wound care, The European Wound Management Association. Recommendations for the management of wound-related symptoms, ewma.org
7. World Health Organisation, Fact sheet Palliativ Care
8. Probst, S., Arber, A., & Faithfull, S. Malignant fungating wounds: The meaning of living in an unbounded body. European Journal of Oncology Nursing.
9. Holistic management of wound-related pain, The European Wound Management Association. ewma.org
10. The benefits of moist wound healing. woundsource.com